Hodgkin Lymphoma | Vibepedia
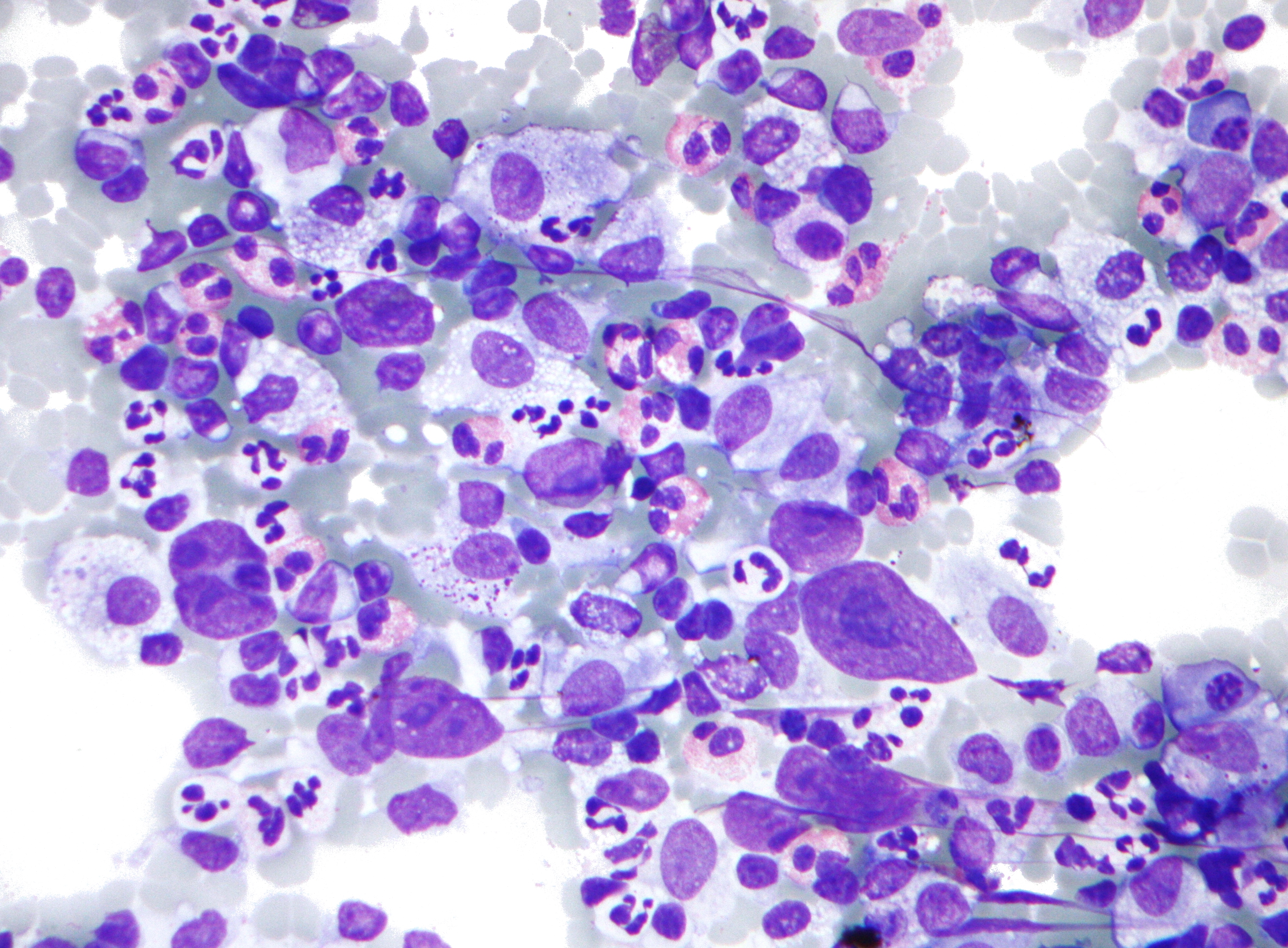
Hodgkin lymphoma (HL) is a distinct type of cancer originating from lymphocytes, a type of white blood cell crucial for the immune system. Its hallmark is the…
Contents
Overview
The story of Hodgkin lymphoma begins in 1832 with the meticulous observations of English physician Thomas Hodgkin. Working at Guy's Hospital in London, he documented a series of patients exhibiting enlarged lymph nodes, spleen, and liver, accompanied by systemic symptoms like fever and wasting. His seminal paper, 'On Some Morbid Appearances of the Absorbent Glands and Spleen,' published in the London Medical Gazette, detailed these cases, though his findings were largely overlooked by his contemporaries. It wasn't until the late 19th century that Samuel Wilks, also at Guy's Hospital, resurrected and popularized Hodgkin's work, formally naming the condition 'Hodgkin's disease' in 1865. This delayed recognition meant that for decades, the disease was poorly understood, with early treatments offering little hope. The subsequent identification of the characteristic Reed-Sternberg cells by Dorothy Reed in 1898 and Albrecht Claus Sternberg in 1907 provided a crucial diagnostic marker, paving the way for more targeted research and understanding of its unique pathology compared to other lymphomas.
⚙️ How It Works
Hodgkin lymphoma arises from a specific type of white blood cell called a B-lymphocyte, a key component of the immune system. The defining feature of HL is the presence of abnormal, large, multinucleated cells known as Reed-Sternberg cells, which are believed to be malignant B-cells. These cells are typically found within a reactive inflammatory background of normal immune cells, including T-lymphocytes, eosinophils, and plasma cells. The disease primarily affects the lymph nodes, but can spread to other lymphoid tissues and organs, including the spleen, liver, and bone marrow. The uncontrolled proliferation of these abnormal cells disrupts normal immune function and can lead to the characteristic symptoms of HL. The two main subtypes, classical Hodgkin lymphoma (cHL) and nodular lymphocyte-predominant Hodgkin lymphoma (NLPHL), differ in the appearance of the malignant cells and their surrounding environment, influencing treatment strategies and prognosis. The role of Epstein-Barr virus (EBV) is significant, particularly in cHL, where it's found in the tumor cells of about 40-50% of cases, suggesting a viral trigger in lymphomagenesis.
📊 Key Facts & Numbers
Globally, Hodgkin lymphoma affects approximately 70,000 people annually, with around 9,000 new cases diagnosed each year in the United States alone. The incidence rate is about 0.3% of all new cancer cases worldwide. HL exhibits a bimodal age distribution, with a peak in young adulthood (ages 15-30) and a second, smaller peak in individuals over age 55. Survival rates are remarkably high; the 5-year relative survival rate for all stages combined in the U.S. is approximately 89%, according to National Cancer Institute data from 2013-2019. For localized HL, the 5-year survival rate approaches 94%, while for distant stages, it's around 84%. The economic burden is substantial, with the average cost of treatment for HL in the U.S. often exceeding $100,000 per patient, encompassing chemotherapy, radiation, and supportive care. Approximately 10-15% of HL cases are the nodular lymphocyte-predominant subtype, which generally has a more indolent course.
👥 Key People & Organizations
The medical and scientific community has been shaped by numerous key figures in understanding and treating Hodgkin lymphoma. Thomas Hodgkin laid the foundational groundwork with his 1832 description. Dorothy Reed's crucial identification of the Reed-Sternberg cell in 1898 provided the diagnostic cornerstone. Later, Henry Kugel and Henry Kugel's work in the mid-20th century was instrumental in developing effective chemotherapy regimens. The Lymphoma Research Foundation and the Leukemia & Lymphoma Society are major non-profit organizations that fund research and provide patient support. Pharmaceutical giants like Bayer AG and Merck & Co. have developed critical chemotherapeutic agents, while newer players like AbbVie and Seagen are at the forefront of immunotherapy and antibody-drug conjugate development for relapsed or refractory HL. The National Cancer Institute (NCI) plays a pivotal role in funding clinical trials and advancing research in the U.S.
🌍 Cultural Impact & Influence
Hodgkin lymphoma's impact extends beyond clinical outcomes, influencing medical education, patient advocacy, and public perception of cancer. The success of treatment regimens, particularly the development of combination chemotherapy like ABVD (Adriamycin, Bleomycin, Vinblastine, Dacarbazine) in the 1970s, became a paradigm for cancer treatment strategies, demonstrating that aggressive, multi-drug approaches could achieve high cure rates for previously fatal diseases. The disease's prevalence in young adults has fostered a strong patient advocacy movement, with organizations like the Lymphoma Research Foundation raising awareness and funds, and advocating for improved access to care and research. The narrative of HL as a 'curable' cancer, especially in its early stages, has offered a beacon of hope and influenced how society views cancer survivorship, often highlighting the resilience of patients and the power of medical innovation. This has also spurred advancements in survivorship care, addressing long-term side effects of treatment.
⚡ Current State & Latest Developments
The current landscape of Hodgkin lymphoma treatment is rapidly evolving, moving beyond traditional chemotherapy and radiation. In 2018, the U.S. Food and Drug Administration (FDA) approved brentuximab vedotin (Adcetris), an antibody-drug conjugate targeting the CD30 protein found on HL cells, for patients with relapsed or refractory disease. More recently, immunotherapy agents like nivolumab (Opdivo) and pembrolizumab (Keytruda), which work by blocking PD-1 receptors to unleash the immune system against cancer cells, have shown remarkable efficacy in treating relapsed/refractory classical HL. These advancements are leading to a paradigm shift, with a growing focus on personalized medicine and de-escalation of therapy in certain patient groups to minimize long-term toxicities. Clinical trials are actively exploring novel combinations, including CAR T-cell therapy and other targeted agents, aiming to further improve cure rates and reduce treatment burden, particularly for patients who do not respond to initial therapies or who relapse.
🤔 Controversies & Debates
A significant debate surrounds the optimal treatment intensity for early-stage Hodgkin lymphoma. While aggressive chemotherapy and radiation offer high cure rates, they also carry substantial long-term risks, including secondary cancers, cardiovascular disease, and infertility, especially in young patients. This has fueled research into 'de-escalation' strategies, aiming to reduce treatment intensity for low-risk patients without compromising efficacy. Conversely, for patients with relapsed or refractory disease, the debate centers on the sequence and combination of novel agents like brentuximab vedotin and immunotherapy. Questions persist about the long-term durability of these newer treatments and their cost-effectiveness compared to established protocols. Furthermore, the precise role of Epstein-Barr virus in HL pathogenesis, and whether its presence can predict treatment response or guide therapy, remains an active area of investigation and discussion among researchers.
🔮 Future Outlook & Predictions
The future of Hodgkin lymphoma treatment is poised for further refinement and personalization. Advances in genomic profiling of HL tumors are expected to identify new therapeutic targets and stratify patients more accurately for treatment. The integration of [[immunotherapy|immunothera
Key Facts
- Category
- science
- Type
- topic